Protecting water safety babies depend on is one of the most important parts of creating a healthy home environment. Infants, young children, pregnant people, older adults, and people with weakened immune systems can all be more vulnerable to contaminants in drinking water than healthy adults. But babies are often the most sensitive group of all. Their bodies are smaller, their organs are still developing, and the amount of water they consume relative to body weight can be surprisingly high, especially when formula is prepared with tap water. That means even low-level contamination that might not immediately affect a healthy adult can be more significant for an infant. Understanding how to assess water quality, what to test for, how to interpret results, and when to take action is essential for parents and caregivers who want a practical, evidence-based approach to safer drinking water.
This article explains the science and the everyday decisions behind infant water safety. It covers why babies are more susceptible, which contaminants matter most, how public water and private well water differ, when and how to test, what results mean, and what steps can reduce risk. The goal is not to create alarm, but to replace uncertainty with clear, actionable knowledge grounded in drinking-water science and public health guidance.
Why babies and other sensitive groups need special attention
Water is fundamental to life, but water quality is not uniform across all homes, communities, or sources. Municipal water systems in many countries are regulated and routinely monitored, yet contamination can still occur in distribution systems, household plumbing, or during local treatment failures. Private wells are not regulated in the same way and often require direct owner responsibility for testing and maintenance. For babies, these differences matter.
An infant’s physiology helps explain why water quality babies rely on deserves special scrutiny:
- Higher intake per body weight: Infants consume more water per kilogram of body weight than adults, whether directly, through formula, or through foods prepared with water.
- Developing organs: The brain, kidneys, liver, immune system, and gastrointestinal system are still maturing, which can increase vulnerability to chemical and microbial contaminants.
- Limited metabolic reserve: Babies may have less ability to tolerate dehydration, gastrointestinal illness, or contaminants that interfere with oxygen transport or nutrient balance.
- Longer life horizon: Early-life exposure to some contaminants can be important because developmental windows are sensitive and cumulative exposures may matter over decades.
Other sensitive groups also deserve attention: pregnant people, because contaminants can affect maternal health and fetal development; immunocompromised individuals, because microbial pathogens can be more severe; and older adults or people with kidney disease, who may be more affected by certain minerals or toxic metals. Still, when families ask whether drinking water should be tested, the presence of a baby in the home is one of the strongest reasons to answer yes.
What “safe water” means in practice
Safe drinking water is not simply water that looks clear, tastes fine, or has no odor. Many of the most important contaminants are invisible, tasteless, and odorless. Lead, arsenic, nitrate, PFAS, and certain microbes may be present even when water seems normal. Public health agencies define drinking water safety through standards, action levels, treatment techniques, and health-based guidelines. These vary somewhat by jurisdiction, but in the United States the U.S. Environmental Protection Agency regulates public drinking water under the Safe Drinking Water Act. Families can review the broader regulatory framework through the EPA drinking water program.
For parents concerned about bottles, formula, and kitchen tap use, the practical meaning of safety is this: water should be low enough in harmful contaminants that routine consumption and food preparation are not expected to cause illness or increase health risk. Because babies are especially sensitive, households often need a more precautionary approach, particularly when the water source is a private well, the plumbing is old, or there has been any known issue with local water quality.
If you are still trying to understand your baseline risk, a good starting point is learning how to know if your tap water is safe to drink. For families with infants, however, a general overview should usually be followed by source-specific testing or review of local water reports.
The scientific background: why infants are more vulnerable to water contaminants
Water contaminants affect the body through different mechanisms. Some are acute hazards that can trigger rapid illness, such as bacteria, viruses, and protozoa that cause diarrhea or vomiting. Others are chronic hazards, such as metals or industrial chemicals that may build exposure over time. Babies can be uniquely sensitive to both categories.
Immature gastrointestinal and immune defenses
Microbial contamination is particularly important for infants because their immune systems are still developing. Pathogens such as E. coli, Salmonella, Campylobacter, norovirus, and Cryptosporidium can cause more severe dehydration and complications in babies than in healthy adults. Even short-term gastrointestinal illness can become medically important more quickly in infants because their fluid balance is less stable.
Kidney development and solute handling
Infant kidneys are less mature than adult kidneys, affecting how babies handle nitrate, sodium, and other dissolved substances. This is one reason nitrate is such a major concern for babies. Excess nitrate can contribute to methemoglobinemia, sometimes called “blue baby syndrome,” a condition in which oxygen delivery in the blood is impaired. Infants younger than about six months are generally considered the highest-risk group.
Neurological sensitivity
Lead is a classic developmental toxicant. No amount of lead exposure is considered beneficial, and even relatively low exposure can affect neurodevelopment. In infants and children, lead exposure has been associated with impacts on learning, behavior, and development. Water is not always the largest lead source overall, but when present, it can be a meaningful contributor, especially for formula-fed infants. This makes water testing infants may consume especially relevant in older homes or areas with legacy plumbing.
Body size and dose
Toxicology often comes down to dose relative to body mass. If a contaminant is present at a fixed concentration in water, a baby consuming that water receives a larger dose per kilogram than an adult drinking the same water. This does not mean every contaminant will cause harm at low levels, but it does mean that risk assessment for infants often needs more caution.
Key contaminants that matter most for infant water safety
Many drinking-water contaminants exist, but some deserve priority because of their relevance to babies and other sensitive groups. The most important categories include microbial hazards, nitrate and nitrite, lead and copper, arsenic, disinfection byproducts, sodium in some contexts, manganese, and emerging contaminants such as PFAS.
1. Microbial contamination
Microorganisms are often the most immediate hazard because they can cause acute illness. Public water systems disinfect water, but contamination can still occur due to treatment failures, main breaks, pressure loss, storage issues, or building plumbing problems. Private wells are especially vulnerable to contamination from septic systems, surface runoff, flooding, animal waste, or poor well construction.
Common microbiological tests include:
- Total coliform bacteria: An indicator of sanitary integrity. Presence suggests a pathway for contamination.
- E. coli: A stronger indicator of fecal contamination and urgent risk.
- Enterococci or other indicators: Sometimes used in source-specific investigations.
For babies, water with confirmed E. coli contamination should not be used for drinking, formula preparation, or food preparation without appropriate emergency guidance and corrective action.
2. Nitrate and nitrite
Nitrate is a top priority in homes with private wells, agricultural runoff influence, septic proximity, or shallow groundwater sources. The EPA maximum contaminant level (MCL) for nitrate in public drinking water is 10 mg/L as nitrogen (often written as nitrate-N), and for nitrite it is 1 mg/L as nitrogen. These limits are particularly protective because of infant risk. High nitrate is one of the clearest examples of water contamination infants are less able to tolerate.
Nitrate is colorless, odorless, and tasteless. Boiling does not remove it; in fact, boiling can concentrate it because water evaporates while nitrate remains. That is a critical point for formula preparation.
3. Lead
Lead usually enters water not from the source water itself, but from corrosion of plumbing materials such as lead service lines, lead solder, and some brass fixtures. Water can pick up lead as it sits in pipes, especially when water is corrosive. Formula mixed with lead-contaminated tap water can significantly contribute to infant exposure.
Lead testing is often most informative when it reflects the actual water people drink, including first-draw or stagnation samples and sometimes flushed samples. Families in older housing stock should learn more about testing lead in water, because the correct sampling method matters.
4. Copper
Copper can also leach from plumbing. It is an essential nutrient, but too much copper can cause gastrointestinal symptoms and may be more concerning for sensitive individuals. Elevated copper can also be a sign of corrosive water chemistry that increases concern for lead and other plumbing-related metals.
5. Arsenic
Arsenic is usually a groundwater issue rather than a plumbing issue and is more common in some geological regions. It is associated with long-term health risks, including cancer and other systemic effects. While immediate infant toxicity is not usually the main framing, early-life exposure is undesirable and worth identifying, especially for private wells.
6. Manganese
Manganese is not always tested in routine panels, but it can matter for infants, particularly in well water. At high levels it can cause taste, staining, and infrastructure problems, and there is ongoing concern about neurological effects from elevated exposure. Water used regularly for infant formula should be checked if manganese is suspected or regionally common.
7. Sodium and total dissolved solids
Sodium is not generally a universal drinking-water contaminant issue, but it can be relevant for certain medically sensitive individuals and in softened water systems. Water softeners that exchange calcium and magnesium for sodium may raise sodium concentrations. For most healthy individuals this is not a major issue, but families preparing infant formula may want to discuss high-sodium water with a pediatric clinician or use an alternate water source if sodium is substantially elevated.
8. Disinfection byproducts and chlorine-related concerns
Public water systems often use chlorine or chloramine to control microbial risks. This is an important public health measure. However, disinfectants can react with organic matter to form byproducts such as trihalomethanes and haloacetic acids. These are regulated in public systems because long-term exposure matters. For infants, the greater immediate risk in many settings is still microbial contamination rather than the presence of a properly maintained disinfectant residual, but it is reasonable to review local consumer confidence reports for these parameters.
9. PFAS and other emerging contaminants
PFAS are a group of persistent synthetic chemicals found in some water supplies. Scientific understanding and regulation are evolving. Because they can persist in the body and environment, families may choose to test for PFAS in areas with known industrial, military, landfill, or firefighting foam impacts. These are not the first contaminants every household must test, but they can be highly relevant in specific regions.
Where risk comes from: source water, treatment, and home plumbing
When parents think about unsafe water, they often imagine a contaminated reservoir or polluted well. But risk can enter at several stages:
- Source water contamination: Agricultural runoff, industrial pollution, naturally occurring metals, septic leakage, or stormwater impacts.
- Treatment limitations: A public system may meet standards overall but still experience temporary issues, seasonal changes, or localized operational challenges.
- Distribution system problems: Water main breaks, pressure loss, biofilm, corrosion, or aging pipes.
- Household plumbing: Lead service lines, copper pipes, brass fixtures, stagnation in pipes, dead-end plumbing, old faucets, or filters that are not maintained.
- Point-of-use storage and handling: Dirty bottle-prep equipment, poorly maintained refrigerator dispensers, faucet aerators, or improper storage of boiled water.
This is why a municipal water report alone does not always answer every question about drinking water safety children need at home. City water can leave the treatment plant compliant and still pick up contaminants in the final stretch before it reaches a bottle in your kitchen.
Public water versus private wells: what changes for families with babies
Public water systems
If your home is served by a public water system, the utility is required to monitor regulated contaminants and provide public reporting. In the United States, this usually comes through an annual Consumer Confidence Report. These reports are useful, but they have limitations:
- They report system-wide results, not always your specific tap.
- They may not capture contamination from your building plumbing.
- Some contaminants are sampled periodically rather than constantly.
- Lead results in utility reports do not directly tell you what is in your child’s bottle water at your faucet.
Parents should also pay attention to boil water notices, service line replacement notices, discolored water events, and local advisories. The CDC healthy drinking water guidance offers practical public health information for households.
Private wells
Private wells carry a very different responsibility profile. They are not typically regulated like public systems, which means the homeowner is responsible for testing, treatment, and maintenance. For households with an infant, that responsibility should be taken seriously and proactively.
Well owners should routinely test for bacteria, nitrate, and regionally relevant contaminants such as arsenic, manganese, uranium, or PFAS where appropriate. Flooding, nearby agricultural activity, septic issues, recent repairs, unusual taste or odor, or a new baby in the home are all strong reasons to test promptly.
Families who rely on wells or who want a broader lab strategy can review how to test drinking water with a complete guide to water testing and analysis and then tailor the panel to infant-specific concerns.
When should you test water if you have a baby?
Testing is not just for emergencies. Ideally, families should think in terms of baseline testing, event-based testing, and periodic retesting.
Baseline testing
Test before a baby is born if possible, or as soon as you begin preparing formula or using tap water for infant foods. Baseline testing is especially important if:
- You use a private well.
- Your home was built before lead plumbing restrictions took effect.
- You have an older service line or unknown plumbing materials.
- You notice staining, metallic taste, sulfur odor, or sediment.
- Your home has been vacant and water has stagnated.
- You live in an agricultural or industrial area.
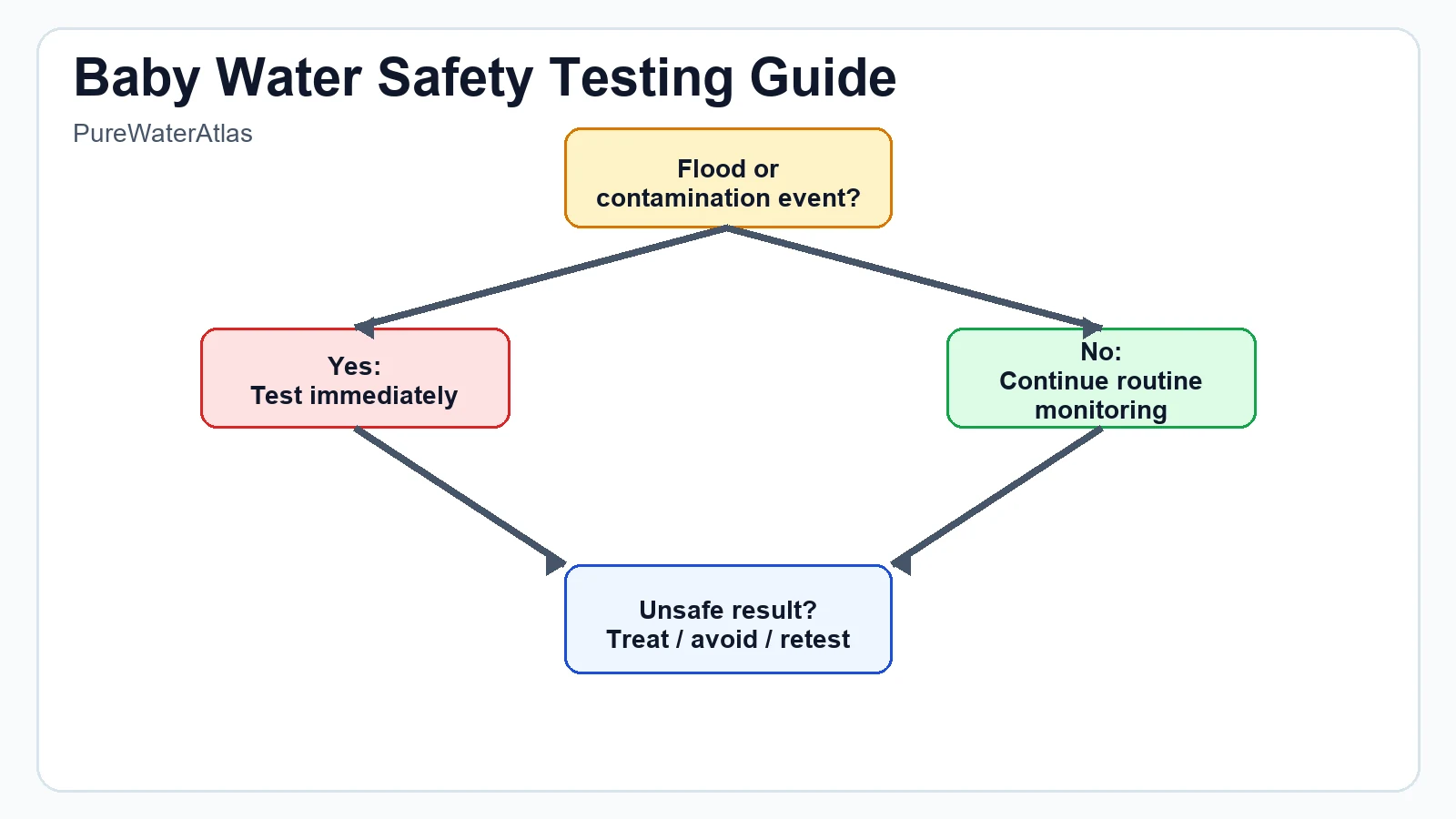
Event-based testing
Test again after changes or incidents such as:
- Flooding or heavy storm runoff
- Well repairs, pump replacement, or disinfection
- Plumbing renovations or faucet replacement
- A water main break or pressure loss event
- New contamination reports in your area
- A boil water notice or suspected microbial event
Periodic retesting
Even if prior results were acceptable, water quality can change over time. Annual testing is a common starting point for private wells, with bacteria and nitrate often emphasized. Public-water households may not need the same full annual testing regimen, but lead testing, targeted contaminant testing, or repeat testing after plumbing changes can be very reasonable where infants are concerned.
What to test for: practical panels for families with infants
The right testing panel depends on your water source and risk profile. A focused strategy is more useful than random testing.
Minimum practical panel for a private well with a baby in the home
- Total coliform and E. coli
- Nitrate and nitrite
- Lead
- Copper
- Arsenic, if regionally relevant
- Manganese, if regionally relevant or if staining/taste issues exist
- pH and general mineral profile if corrosion or treatment decisions are relevant
Suggested targeted panel for public-water households with infants
- Lead
- Copper
- Optional first-draw and flushed comparisons
- Nitrate if there is a source-specific concern or mixed source
- Bacteria testing if there has been a household plumbing issue, storage issue, or suspected contamination event
Urban homes with older plumbing may need a more location-specific approach; this is especially true in apartment buildings or neighborhoods with legacy infrastructure. In such cases, guidance on tap water testing in urban homes can help families identify plumbing-related risk factors.
How water testing works: home kits, strips, and certified laboratories
Not all tests offer the same reliability or purpose. Understanding the differences helps parents make better decisions.
DIY test strips
Test strips can be useful for rough screening of parameters like nitrate, hardness, pH, or chlorine, but they are limited. They are generally not the best choice for confident decision-making about infant exposure, especially for lead, arsenic, or microbial contamination.
Mail-in lab kits
Mail-in kits can be a practical middle ground when they use certified laboratories and provide clear sampling instructions. These are often useful for lead, bacteria, nitrate, and common metals. The quality depends on the lab and the sampling process.
State-certified or accredited laboratory testing
For the highest confidence, especially when making decisions for a baby, certified laboratory testing is preferred. This matters because collection method, preservation, timing, chain of custody, and analytical method all affect result quality.
For example:
- Lead: The sample may need to be collected after a period of stagnation to capture worst-case exposure at the tap.
- Bacteria: Sterile bottles, correct fill volume, and prompt submission are essential.
- Nitrate: Proper preservation and timely analysis help ensure valid results.
How to collect a useful sample
Water test results are only as good as the sample. Parents frequently make sampling mistakes that create false reassurance or unnecessary concern.
General rules
- Follow laboratory instructions exactly.
- Sample from the faucet actually used for drinking or formula preparation.
- Do not sample through a dirty filter, removable hose, or contaminated container unless the lab instructs otherwise.
- Record whether the sample is first-draw, flushed, or post-treatment.
- Label samples carefully and submit them within required time windows.
For lead testing
Lead sampling often intentionally captures water that has sat in plumbing. That means sampling after water has remained unused for a defined period, commonly several hours. This reflects potential exposure from water that has been in contact with pipes overnight or during the day. A flushed sample may also be taken to compare how much the plumbing versus the supply contributes.
For bacteria testing
Bacteria samples typically require a sterile bottle provided by the lab. Touching the inside of the cap, rinsing the bottle, or using an unclean faucet can invalidate the sample. Sometimes the faucet is disinfected or aerators removed before collection, depending on test purpose.
How to interpret results for babies and sensitive groups
Interpreting water results is not just a matter of “pass” or “fail.” Some contaminants have legal limits, some have health-based goals, and some have aesthetic benchmarks related to taste or staining rather than direct health. For infant use, conservative interpretation is often appropriate.
| Contaminant | Why it matters for infants | Practical interpretation point |
|---|---|---|
| E. coli | Indicates fecal contamination and acute infection risk | Do not use for drinking or formula until corrected and confirmed safe |
| Total coliform | Indicates possible pathway for contamination | Investigate source and retest; significance depends on context |
| Nitrate | Associated with infant methemoglobinemia risk | At or above regulatory concern warrants alternative water or treatment |
| Lead | Developmental neurotoxicant | Any detectable lead deserves attention, especially for formula use |
| Copper | Can indicate corrosive plumbing and may cause GI upset | Evaluate with plumbing context and corrosion factors |
| Arsenic | Long-term toxicant with chronic health concerns | Persistent elevation requires treatment or alternate source |
| Manganese | May be relevant at elevated levels in infant water | Assess especially for wells and formula use |
When reviewing numerical values, compare them with authoritative drinking-water standards and context-specific guidance. A helpful reference point is understanding safe water levels for common contaminants, but parents should remember that a regulatory limit is not always the same thing as an ideal target for infant exposure.
What to do if the water test shows a problem
The right response depends on the contaminant. Some problems demand immediate use changes, while others allow for planned corrective action. If your results raise concern, avoid guesswork. Document the findings, confirm whether the sample was collected properly, and choose a response that matches the contaminant.
Immediate-response situations
- E. coli positive: Stop using the water for drinking, formula, and food preparation until the problem is corrected and follow-up testing confirms safety.
- High nitrate: Do not rely on boiling. Use an alternate safe water source for infant feeding until treatment or source correction is in place.
- Elevated lead at the tap: Use an alternate source or a filter certified for lead reduction at the relevant tap while investigating plumbing and long-term correction.
Corrective options
- Shock chlorination or sanitary repairs for bacterial well contamination
- Well reconstruction, casing repair, or relocation of contamination sources
- Point-of-use reverse osmosis or specialized treatment for nitrate, arsenic, and some other dissolved contaminants
- Certified lead-removal filters, corrosion control measures, or plumbing replacement for lead and copper
- Alternate bottled water as a temporary measure when appropriately chosen and stored
If you need a structured response plan after a bad result, see what to do if your water test fails. The key is to match the solution to the contaminant rather than assuming one filter or one home remedy fixes everything.
Can you just boil water for infant safety?
Boiling is useful for some microbial emergencies, but it is not a universal fix. It may reduce infection risk during some contamination events, but it does not remove lead, nitrate, arsenic, PFAS, or most dissolved chemicals. In the case of nitrate, boiling can worsen concentration. This is one of the most common misconceptions around water safety babies depend on. Parents should only use boiling when it is recommended for a specific microbial concern and should understand its limits.
Choosing treatment systems for infant-safe water
Treatment decisions should be based on test results, not marketing claims. Different technologies address different contaminants:
- Activated carbon: Can reduce chlorine, taste, odor, and some organic chemicals, depending on design. Not reliable for nitrate and not universally effective for metals.
- Reverse osmosis: Often effective for nitrate, arsenic, many dissolved contaminants, and some PFAS, but performance depends on system design and maintenance.
- Ion exchange: Can treat nitrate or hardness in specific configurations.
- Distillation: Can remove many dissolved contaminants, but practicality varies.
- UV disinfection: Addresses microbes when properly sized and maintained, but does not remove chemicals.
For households with babies, point-of-use systems at the kitchen tap used for formula preparation are often the most practical. Whatever system is chosen, verify that it is certified for the specific contaminant of concern, installed correctly, and maintained on schedule. A neglected filter can fail or even become a microbial growth site.
Formula preparation and safe water handling
Water testing is only part of infant exposure prevention. How water is handled also matters.
- Use water from a tested, trusted source for mixing formula.
- If using a treatment system, use the treated tap consistently for infant feeding.
- Clean bottle-preparation surfaces, containers, and equipment thoroughly.
- Do not store prepared formula longer than recommended by healthcare guidance.
- Do not assume refrigerator water dispensers or pitcher filters remove infant-relevant contaminants unless certified to do so.
- Replace filter cartridges on time.
The World Health Organization provides broader public-health context on safe drinking water and contamination risk through its drinking water fact sheet, which is helpful for understanding why contamination prevention and treatment remain global health priorities.
Regional and environmental factors that influence water risk
Not every household needs the same testing panel because local geology, infrastructure, and land use shape water quality patterns. Examples include:
- Agricultural regions: Higher concern for nitrate, pesticides, and well contamination.
- Older cities: Higher concern for lead service lines and aging plumbing.
- Mining or naturally mineralized regions: Arsenic, manganese, uranium, or iron may be more relevant.
- Flood-prone areas: Greater episodic microbial contamination risk.
- Industrial corridors or military-adjacent zones: PFAS and industrial solvents may warrant evaluation.
Parents can gain additional perspective on local groundwater and hydrology through the USGS water resources information, especially when trying to understand how regional conditions might affect private wells.
Common misconceptions about water quality for babies
- “If the water is clear, it is safe.” False. Many dangerous contaminants are invisible.
- “My city water report says the water is fine, so my baby’s bottle water is fine.” Not always. Household plumbing can change the picture.
- “Boiling makes any water safe.” False for many chemicals and metals.
- “A basic pitcher filter removes everything.” False. Filters vary enormously by contaminant.
- “Only well owners need testing.” False. Public-water homes may still need tap-specific lead or plumbing-related testing.
- “If adults are not getting sick, the baby is not at risk.” False. Infants have different vulnerabilities and dose patterns.
Practical checklist for parents and caregivers
- Identify your water source: public system or private well.
- Review local water reports if on public water.
- Test tap water used for formula or infant foods if plumbing is old or unknown.
- For wells, test at minimum for bacteria and nitrate, then expand based on local risks.
- Do not rely on taste, smell, or appearance as proof of safety.
- Use certified treatment only for contaminants confirmed or strongly suspected.
- Retest after repairs, contamination events, flooding, or major plumbing work.
- Keep records of all results and treatment maintenance.
FAQ
Should I test tap water before using it for baby formula?
Yes, especially if you use a private well, live in an older home, have unknown plumbing materials, or have any reason to suspect contamination. Lead, nitrate, and bacteria are among the most important concerns depending on the source.
Is bottled water always safer for babies?
Not automatically. Bottled water quality varies, and not all bottled water is ideal for formula preparation. It can be a useful temporary alternative during contamination problems, but it should come from a reputable source and be used with attention to storage and hygiene.
What is the most important contaminant to test for in well water for infants?
There is no single answer, but bacteria and nitrate are usually top priorities. Regional contaminants such as arsenic or manganese may also be very important.
Can a faucet filter make water safe for a baby?
Sometimes, but only if the filter is certified for the specific contaminant present and is properly maintained. A general taste-and-odor filter may not remove lead, nitrate, or microbes.
How often should well water be tested when there is a baby in the home?
Annual testing is a common minimum for bacteria and nitrate, with additional testing after flooding, repairs, contamination events, or any major change in water quality.
Conclusion
Ensuring water safety babies depend on is not about perfection or fear. It is about informed prevention. Babies are uniquely sensitive to waterborne microbes, nitrate, lead, and other contaminants because of their size, development, and feeding patterns. The safest approach is to identify your water source, understand the likely risks, test strategically, and respond with contaminant-specific treatment or alternate water when needed. For families, a clear water test and a reliable plan for ongoing monitoring can turn uncertainty into confidence and help protect the people who are least able to protect themselves.
Featured image: Photo by olia danilevich on Pexels.
Read the full guide: Water Testing Guide
Explore more in this category: Water Testing Articles