Bacteria water testing is one of the most important parts of protecting drinking water quality. Unlike many chemical contaminants, bacteria can indicate a direct sanitary problem: fecal pollution, poor well construction, distribution system breaches, inadequate disinfection, or unsafe storage. A positive bacterial result does not always mean severe illness will occur, but it does mean the water source, plumbing, or handling system may be vulnerable to contamination. For households, schools, small systems, and rural well owners, understanding how to test for bacteria in drinking water safely is essential for making sound decisions about risk, treatment, and follow-up action.
Microbial contamination is a public health concern because disease-causing organisms can enter water through sewage, septic system failures, animal waste, stormwater runoff, floodwater, or defects in wells and pipes. Public health agencies including the U.S. Environmental Protection Agency, the Centers for Disease Control and Prevention, and the World Health Organization all emphasize the importance of microbiologically safe drinking water. In practice, most routine drinking water microbiology testing does not attempt to detect every pathogen directly. Instead, laboratories usually test for indicator organisms, especially total coliforms and Escherichia coli, because these bacteria help identify whether contamination has likely entered the water.
This article explains the scientific basis of bacterial testing, the most common test types, how to collect samples safely, how to interpret results, and what steps to take if contamination is found. If you want a broader overview of analytical methods beyond microbiology, PureWaterAtlas also covers how to test drinking water comprehensively. Here, the focus stays on bacteria water testing and the practical steps needed to do it correctly.
What bacteria water testing actually measures
When people ask for a “bacteria test” for drinking water, they are often referring to one of several related analyses. The most common are total coliform, fecal coliform, and E. coli testing. A standard coliform bacteria test does not usually identify every species present in the sample. Instead, it screens for groups of bacteria that signal whether contamination pathways exist. This is scientifically useful because testing directly for all possible waterborne pathogens would be slower, more expensive, and technically more complex.
Total coliform bacteria are widely used as indicator organisms. They are found in soil, vegetation, and the intestines of warm-blooded animals, so a positive result can mean environmental intrusion or poor sanitary integrity. Total coliforms alone do not necessarily prove fecal contamination, but they suggest the water system may not be well protected.
E. coli is a much more specific indicator of fecal pollution. An e coli water test is particularly important because E. coli is strongly associated with contamination from human or animal waste. That matters because if fecal material has entered the water, pathogens such as certain bacteria, viruses, and protozoa may also be present. For a scientific primer on microbial hazards and indicator organisms, see PureWaterAtlas coverage of water microbiology, bacteria, viruses, and microbial risks in drinking water.
Some laboratories also offer heterotrophic plate count testing, enterococci, or fecal streptococci testing. These can be useful in specific contexts, but for routine private well screening and many basic safety checks, total coliform and E. coli are the most common and actionable indicators.
Why bacterial contamination matters for drinking water safety
Water contamination bacteria can lead to mild or severe illness depending on the organism, dose, and the vulnerability of the person exposed. Infants, older adults, pregnant people, transplant recipients, people receiving chemotherapy, and anyone with a weakened immune system may face higher risk from microbiologically unsafe water. Symptoms associated with waterborne infections can include diarrhea, vomiting, abdominal cramps, fever, and dehydration. However, not every contaminated water sample will cause noticeable illness, and not every illness after drinking water can be traced to a water source.
The larger point is preventive: bacteria water testing helps identify problems before they become outbreaks. A contaminated sample may reveal a cracked well cap, surface runoff entering a poorly sealed casing, a failing septic setback, cross-connections in plumbing, loss of disinfectant residual, or contamination introduced during flooding. In public water systems, bacterial monitoring is a cornerstone of regulatory compliance because it helps verify that treatment and distribution barriers remain intact.
Water safety bacteria concerns are especially important for private wells because many private supplies are not monitored by a utility. In those settings, the owner is responsible for sampling, testing, interpreting results, and maintaining sanitary protection. That makes reliable sample collection and laboratory selection crucial.
The scientific basis: indicator organisms versus pathogens
From a microbiological standpoint, testing for pathogens directly is often challenging. Many pathogens are difficult to culture, may occur intermittently, and can be present in low numbers while still posing risk. Sampling volume, transport time, detection method, and laboratory capability all influence the ability to detect them.
Indicator organisms solve part of this problem. An ideal indicator should be present when fecal contamination is present, absent when contamination is absent, detectable by standardized methods, and at least as persistent as the pathogens of concern. No indicator is perfect, but total coliforms and E. coli have strong practical value.
Total coliforms are useful for assessing sanitary integrity. If they appear in a sample, the water system may be open to contamination somewhere. E. coli is more specific for fecal input and generally triggers a stronger response. A positive E. coli result in drinking water is considered an urgent finding because it may indicate recent fecal contamination and potential pathogen presence.
It is also important to understand limitations. A negative result does not mean the water is permanently safe. Microbial contamination can be intermittent, especially after rain, flooding, pump work, power outages, or seasonal groundwater changes. A single clean sample is informative, but repeated testing and context matter. The U.S. Geological Survey provides useful background on groundwater, hydrology, and how environmental conditions can affect source water vulnerability.
Common sources of bacterial contamination in drinking water
Understanding sources helps people test more intelligently and respond more effectively. Common pathways for water contamination bacteria include the following:
- Failing septic systems or leaking sewer infrastructure near a well or source water intake
- Surface water entering a shallow, poorly constructed, or damaged well
- Flooding that submerges a wellhead, spring box, or storage tank
- Animal waste from livestock areas, pastures, wildlife activity, or manure application
- Cracked well casings, loose caps, missing sanitary seals, or improper grading around the well
- Backflow or cross-connections in plumbing systems
- Improperly cleaned cisterns, tanks, or household storage containers
- Disturbance after pump replacement, well rehabilitation, or plumbing repairs
- Distribution system breaks or pressure loss in public or small community systems
Many bacterial contamination events are associated with physical defects rather than mysterious water chemistry. That is why testing should often be paired with inspection of the source, surrounding land use, and plumbing conditions.
When you should test drinking water for bacteria
Routine testing frequency depends on the water source and the level of risk. For private wells, annual testing for total coliform and E. coli is a common minimum recommendation, with additional testing whenever conditions suggest a contamination event. For people who rely on private wells, PureWaterAtlas offers a practical well water testing checklist that helps organize routine and event-based sampling.
You should consider immediate bacteria water testing if:
- The water changes after heavy rain, flooding, or snowmelt
- You notice a damaged well cap, casing, seal, or nearby septic issue
- The well has been serviced, opened, deepened, or disinfected recently
- There has been a plumbing repair, pressure loss, or backflow incident
- You are buying a home with a private water supply
- The water develops unusual turbidity, odor, or color after an event
- Someone suspects gastrointestinal illness linked to the water
- The water source has been inactive for a prolonged period
Emergency sampling may also be needed after disasters. If the source has been flooded or the system has lost integrity, rapid action matters. For that situation, PureWaterAtlas has guidance on emergency water testing.
Main types of bacterial drinking water tests
Total coliform test
A total coliform test checks whether bacteria from the coliform group are present or absent. This is the most common screening test for private wells and many non-emergency drinking water assessments. A positive result suggests that the source or system is not adequately protected. It may reflect environmental intrusion rather than fecal contamination, but it still deserves follow-up.
E. coli water test
An e coli water test is more specific for fecal contamination. Many labs perform a combined total coliform and E. coli analysis from the same sample. If total coliform is present and E. coli is absent, the result suggests sanitary vulnerability without direct evidence of fecal pollution. If E. coli is present, the water should generally be treated as unsafe for drinking until the cause is identified and corrected.
Fecal coliform test
Fecal coliform testing was historically common, but many modern drinking water programs prioritize E. coli because it is a more specific indicator. Some labs still offer fecal coliform testing in environmental, recreational water, or wastewater contexts.
Presence-absence tests
Presence-absence tests report whether target bacteria are detected in a fixed sample volume, often 100 mL. These tests are common for routine potable water screening because they are cost-effective and directly useful for safety decisions.
Quantitative tests
Quantitative methods estimate bacterial concentration, usually as colony-forming units or most probable number per 100 mL. These are useful in some investigations, repeat sampling, and system management contexts.
Heterotrophic plate count
Heterotrophic plate count measures general bacterial growth potential rather than fecal contamination specifically. It can help assess biofilm activity, treatment performance, or distribution system conditions, but it is not a substitute for a coliform bacteria test or E. coli analysis when the goal is drinking water safety screening.
Laboratory methods used in water microbiology testing
Water microbiology testing relies on standardized methods designed to minimize contamination, preserve sample integrity, and detect low-level bacterial presence. The exact method used by the laboratory affects turnaround time and reporting format, but the most common methods fall into a few categories.
Membrane filtration
In membrane filtration, a measured volume of water is passed through a fine membrane that traps bacteria. The membrane is then placed on selective growth media and incubated. If target organisms are present, they form colonies that can be counted and sometimes confirmed by color or further biochemical testing. This method is widely used and can provide quantitative results.
Most probable number methods
Most probable number, often abbreviated MPN, uses multiple test wells or tubes containing selective media. If bacteria grow and produce characteristic reactions, statistical tables estimate the likely concentration. Many modern drinking water bacterial tests use enzyme-substrate media that change color or fluoresce when coliforms or E. coli are present.
Presence-absence bottle tests
Some private well screening programs use single presence-absence containers with specialized media. These are convenient and useful for routine decisions, though the result is qualitative rather than highly quantitative.
Rapid molecular methods
Polymerase chain reaction and related methods can detect microbial genetic material quickly, but they are more common in specialized laboratories, outbreak investigations, research, or source tracking. For routine household drinking water, culture-based or enzyme-substrate indicator tests remain more common.
Home kits versus certified laboratory testing
Many consumers encounter mail-in kits, strip tests, incubator kits, or field bottles advertised for bacteria water testing. Some are useful screening tools, but they are not all equal. The more important the decision, the more important the analytical reliability. For routine health protection, especially when a positive or negative result will drive corrective action, certified laboratory testing is usually the best choice.
Home kits can be helpful when:
- You need a quick screening check after a suspected event
- You live far from a laboratory and need a first-pass assessment
- You understand the method’s limitations and will confirm concerning results
Certified laboratory testing is preferable when:
- You need results for a real estate transaction, regulatory requirement, or formal documentation
- The sample comes from a drinking water well, school, childcare setting, or healthcare-related environment
- You have vulnerable household members
- A previous sample was positive
- You need method-specific interpretation and professional follow-up
The key issue is false confidence. Bacterial testing is highly sensitive to sampling technique, incubation conditions, and container sterility. A poor-quality kit or improper handling can produce misleading results in either direction.
How to collect a drinking water sample safely
Safe and valid sample collection is the foundation of meaningful bacteria water testing. Even a high-quality laboratory cannot fix a contaminated or mishandled sample bottle. The objective is to collect water that truly represents the source or plumbing point you want to evaluate without introducing microbes from hands, sink surfaces, hoses, or containers.
Use the correct sterile container
Always obtain the sample bottle from the laboratory or a trusted provider. The bottle should be sterile and, in many cases, contain sodium thiosulfate if the water is chlorinated. Sodium thiosulfate neutralizes residual disinfectant so bacteria present at the time of sampling are not killed before analysis.
Choose the right tap
Select a cold-water tap that is clean and directly connected to the plumbing you want to test. Avoid swing faucets, leaking faucets, garden hoses, threaded hose bibs if possible, and taps with aerators or screens unless the lab instructs otherwise. A kitchen faucet can be acceptable, but many laboratories prefer a plain indoor tap without attachments because it reduces the chance of contamination from the fixture itself.
Prepare the outlet properly
If instructed, remove aerators, screens, or filters. Clean visible debris. Some protocols call for disinfecting the faucet outlet with alcohol or a dilute bleach solution and then letting the water run for a set time. Others specify flushing without disinfection depending on the goal of the sample. Follow the laboratory instructions exactly, because sampling for source integrity versus distribution or household plumbing may require slightly different approaches.
Wash hands and avoid touching the bottle interior
Wash your hands before sampling. Do not touch the inside of the cap or bottle. Do not set the cap down on a counter. Hold it facing downward or as directed while you fill the bottle.
Flush the line as instructed
Some labs recommend running the cold water for two to five minutes, or until the pump cycles, to obtain a more representative sample of the well or main line. Others may request a first-draw sample if the question involves point-of-use contamination. The lab’s instruction sheet should control the procedure.
Fill the bottle correctly
Open the bottle immediately before collection. Fill to the marked line if present. Do not overfill. The lab may need headspace for mixing. Avoid splashing or rinsing the bottle. Never rinse a sterile microbiology bottle, because doing so destroys the sterile condition and may wash out preservatives.
Keep the sample cool and deliver quickly
Microbiology samples are time-sensitive. Most labs require delivery within a short holding time, often the same day and commonly within 24 hours of collection, with cooling but not freezing during transport. Follow the lab’s chain-of-custody and storage instructions carefully.
Common sampling mistakes that can invalidate results
False-positive and false-negative outcomes often begin with poor sampling technique. The most common problems include:
- Using a non-sterile bottle or opening the sterile bottle too early
- Touching the inside of the bottle or cap
- Sampling from a dirty faucet, hose, or aerator coated with biofilm
- Collecting hot water instead of cold water
- Overfilling or underfilling the bottle
- Failing to use sodium thiosulfate-preserved bottles for chlorinated water
- Delaying transport beyond the allowed holding time
- Leaving the sample warm in a vehicle or direct sunlight
- Ignoring the laboratory’s specific tap preparation instructions
A positive result caused by contamination during collection is frustrating, but it still teaches an important lesson: microbiological analysis is only as good as the procedure. If a result seems inconsistent with the water source or appears borderline in a complicated setting, repeat sampling may be appropriate.
How to interpret bacteria test results
Interpreting bacterial results depends on the method, the sample location, whether the water is public or private, and whether the finding is total coliform only or E. coli positive. Reading the report carefully matters. For more help on report language and lab formats, PureWaterAtlas explains how to understand water test results.
Absent or not detected
If total coliform and E. coli are absent or not detected in the sample volume tested, the result is favorable. It means the lab did not detect those indicator bacteria in that sample. It does not guarantee future safety, but it supports the conclusion that the source was microbiologically acceptable at the time of sampling.
Total coliform present, E. coli absent
This pattern suggests the system may be vulnerable to contamination, though the evidence does not specifically indicate fecal pollution. The problem could be environmental bacteria entering through a well defect, contaminated plumbing fixtures, poor sample collection, or regrowth in some system components. The usual response is to inspect the system, repeat the test, and determine whether corrective action such as sanitization or repair is needed.
E. coli present
If E. coli is present, the water should generally be considered unsafe for drinking until the issue is investigated and corrected. Boiling water may be recommended as an interim protective step depending on public health guidance and the type of system involved. The source should be inspected, the contamination pathway identified if possible, and repeat testing performed after corrective action.
Count-based results
If the lab reports colony-forming units or MPN per 100 mL, any confirmed E. coli in drinking water is cause for concern. For total coliform, count values can help characterize the extent of contamination, but the basic interpretation remains focused on sanitary integrity and follow-up action.
Regulatory context and standards
For treated public drinking water systems, microbial monitoring is governed by regulations and routine compliance frameworks. Standards vary by country and system type, but one central principle is widely shared: E. coli should not be present in drinking water. Regulatory programs often use total coliform and E. coli monitoring to evaluate treatment performance, distribution integrity, and corrective action requirements.
Private wells are usually not regulated in the same way as public systems, yet the health objective is similar: drinking water should be free of fecal indicator bacteria. It is useful to understand the broader framework of acceptable drinking water quality, especially when lab reports reference standards or action levels. PureWaterAtlas provides additional background on water quality standards explained.
One practical caution: regulatory compliance language for utilities should not be confused with household decision-making. A private homeowner does not need a formal violation notice to take a positive E. coli result seriously.
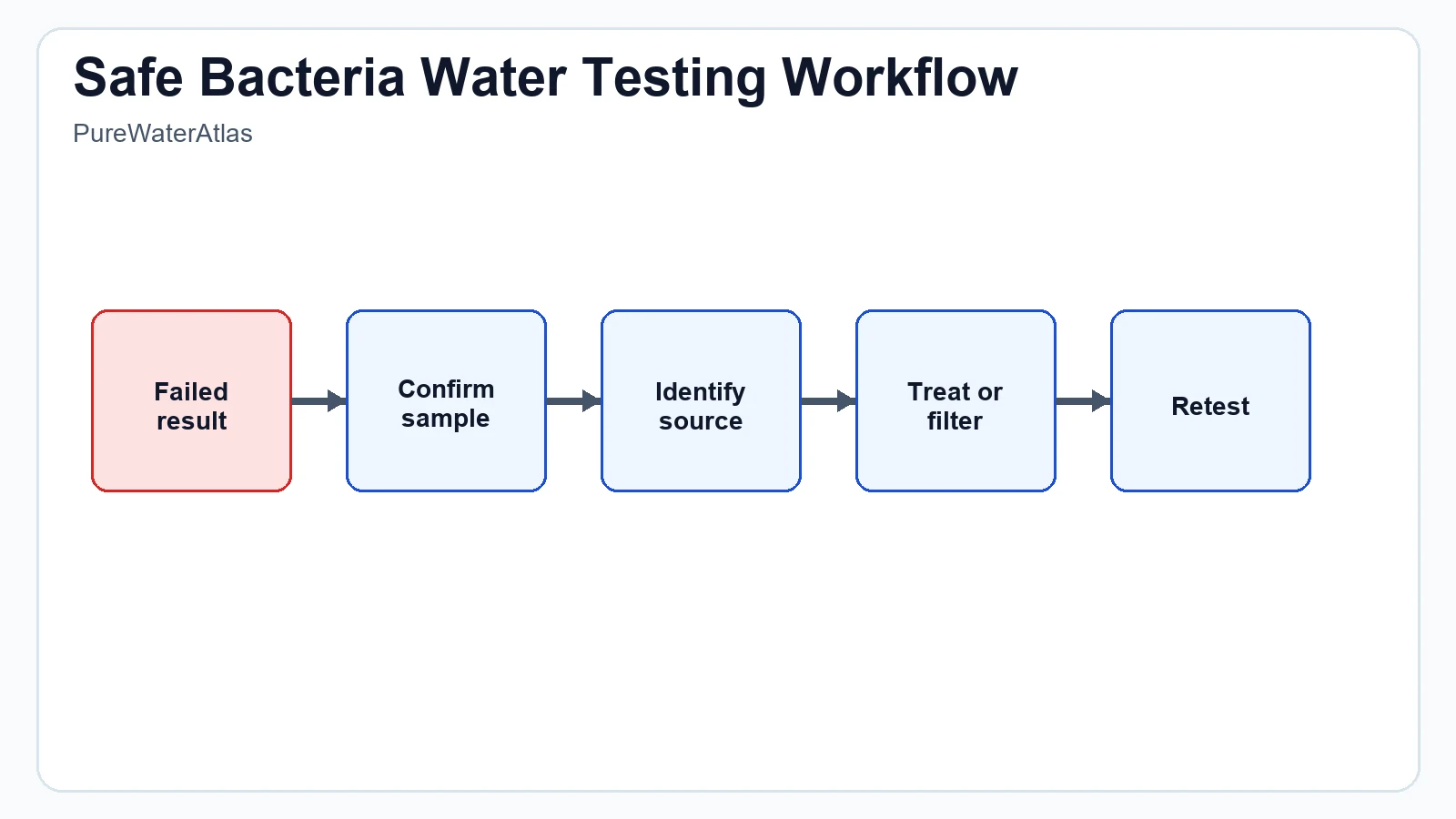
What to do if your sample tests positive
The right response depends on the result and the likely source of contamination, but certain general steps are widely recommended.
If E. coli is detected
- Do not use the water for drinking, brushing teeth, preparing infant formula, washing produce, making ice, or cooking unless you are following safe interim guidance such as boiling where appropriate.
- Inspect the wellhead, cap, casing, nearby septic system, drainage, and any recent disturbance or flood history.
- Contact a qualified laboratory, local health department, water professional, or well contractor for source investigation.
- Disinfect and repair the system as recommended based on the identified cause.
- Retest after corrective action to confirm that contamination has been removed.
If only total coliform is detected
- Repeat the sample, ideally with careful collection technique or professional sampling.
- Inspect for sanitary defects and contamination pathways.
- Consider shock chlorination only if it is appropriate for the system and paired with physical correction of the problem.
- Retest to verify whether the finding persists.
Shock chlorination can temporarily reduce bacteria in a well or plumbing system, but it is not a permanent fix if the source remains vulnerable. If a cracked cap, poor surface grading, or failing sanitary seal allows contamination to re-enter, the bacteria often return.
Long-term prevention of bacterial contamination
The best bacterial control strategy is barrier protection: keep contamination out of the water source and maintain conditions that prevent microbial intrusion. Preventive measures include:
- Maintain proper well construction, sanitary cap integrity, and secure casing seals
- Keep runoff, standing water, and floodwater away from the wellhead through proper grading
- Protect setback distances from septic systems, livestock, and manure storage
- Inspect the well after storms, flooding, or nearby construction
- Disinfect and retest after repairs, pump work, or line replacement when appropriate
- Clean and maintain cisterns, storage tanks, and household point-of-entry systems
- Test routinely, not only after problems become obvious
For some households, treatment may be necessary. Continuous disinfection systems such as ultraviolet treatment or chlorination can reduce microbial risk, but they do not eliminate the need to fix structural vulnerabilities and monitor performance. Treatment should be selected based on the actual contamination pattern, water quality conditions, maintenance capacity, and confirmation testing.
Special situations: wells, springs, cisterns, and post-flood testing
Private wells
Wells are often vulnerable at the surface connection points rather than deep underground alone. A modern, properly sealed well can provide excellent water, but shallow wells, dug wells, or older installations may be much more susceptible to bacterial entry.
Springs and spring boxes
Spring-fed systems can be highly variable and are often at greater risk from direct surface influence. Frequent bacteria water testing may be necessary, especially after storms.
Cisterns and hauled water storage
Stored water can become contaminated during filling, transport, or storage. In these systems, test both the incoming water source and the stored water if bacterial problems are suspected.
After flooding
Floodwater can carry sewage, animal waste, soil bacteria, and debris into wells and storage systems. If the wellhead has been submerged, the system should be considered at risk until it is inspected, disinfected if appropriate, and retested. Flood-related contamination is a classic situation where water safety bacteria concerns become urgent.
How often should private well owners test?
At a minimum, annual bacteria water testing is a prudent baseline for most private wells. Additional testing is advisable after any event that could affect sanitary integrity. In higher-risk settings, more frequent testing may be reasonable, such as:
- Seasonal homes reopening after closure
- Shallow wells in agricultural areas
- Properties with a history of positive coliform results
- Wells affected by storm runoff or flooding
- Homes with infants or immunocompromised occupants
If a household has recurring contamination, periodic screening alone is not enough. The source of intrusion needs to be identified and corrected, or an appropriate continuous treatment system needs to be installed and maintained.
FAQ
What is the best bacteria test for drinking water?
For most households, a total coliform and E. coli test performed by a certified laboratory is the most useful routine screening option. It is practical, scientifically established, and directly relevant to drinking water safety.
Can I trust a home bacteria water testing kit?
Some home kits are useful for screening, but reliability varies. For important health decisions, recurring problems, or documentation needs, certified laboratory testing is usually the better choice.
How long do bacteria test results take?
Many standard coliform bacteria test methods take about 18 to 48 hours after the lab receives the sample, though exact timing depends on the method and the laboratory.
What does it mean if total coliform is present but E. coli is not?
It usually means the water system may be vulnerable to contamination, but the test does not show direct evidence of fecal contamination in that sample. Repeat testing and system inspection are commonly recommended.
Is any E. coli acceptable in drinking water?
No. E. coli in drinking water is generally treated as an unacceptable result and requires prompt follow-up and corrective action.
Should I boil water if bacteria are found?
If E. coli or fecal contamination is suspected, boiling may be used as an interim measure when consistent with local public health guidance. However, boiling is not a substitute for identifying and correcting the contamination source.
Conclusion
Safe bacteria water testing is not just about sending a bottle to a lab. It requires understanding what is being tested, using proper sterile sampling technique, interpreting the result in context, and taking meaningful action when contamination is found. A good coliform bacteria test or e coli water test can reveal hidden sanitary problems long before they become obvious. For private well owners and anyone responsible for drinking water safety, that makes routine water microbiology testing one of the most valuable preventive tools available. When the sampling method is sound and the results are followed by inspection, repair, retesting, and prevention, bacterial testing becomes far more than a checklist item: it becomes a practical safeguard for public health.
Read the full guide: Water Testing Guide
Explore more in this category: Water Testing Articles